Breastfeeding/Chestfeeding- Common Questions
Updated December 28th, 2023

You may have some questions about breastfeeding/chest feeding. Find the answers to some frequently asked questions below.
What is triple feeding?
Triple feeding is when you do three things to feed your baby – feed at the breast, express milk by pumping and feed the expressed milk or formula to your baby. It is meant to be a temporary measure to increase breast milk supply and help babies gain weight. If you need help to breastfeed more, check out our breastfeeding resources.
Why is paced feeding important?
Paced feeding is a method of bottle feeding that mimics feeding at the breast. Holding the baby upright and the bottle parallel to the ground ensures a slower milk flow out of the bottle. If the baby pauses to breath or because they are full, you can tilt the bottle down.
Paced feeding
- protects direct breastfeeding
- prevents using up more breastmilk stash or formula than needed
- prevents overfeeding the baby.
Watch this video to learn how to feed your baby with a paced bottle.
Note: Other videos may be recommended by the host channel (e.g. YouTube, Vimeo). These suggestions may be based on your personal search history and other factors. The WRHA does not control these suggestions and is not responsible for and may not endorse the content.
Do I need a special bra?
- Not everyone finds that a maternity or nursing bra is necessary. Some breast/chest feeding parents just use an inexpensive and comfortable sports bra.
- Nursing bras have clasps or panels that allow easy access to your breasts for breastfeeding.
- For comfort, choose a bra with wide straps, extra hooks and eyes on the band, comfortable breathable material (such as cotton).
- Wear a comfortable and supportive bra that is not too tight. Avoid underwire bras as they can block your milk ducts.
- On average, you can expect to go up one cup size, and one band size, by the time you are breastfeeding.
Hot parent tip:
- You may leak breast milk in between feedings. Breast pads can help absorb the milk. You can find breast pads in the baby section at most stores.
- Be sure to change wet breast pads often so they don’t grow bacteria which can lead to thrush. See below for more information on thrush.

Are sore nipples common?
- It’s common to feel some pain when your baby latches on for the first few days. This happens because your baby stretches your nipple deep into their mouth while breastfeeding and your body is not used to this sensation. The pain happens when the baby first latches on and should go away within a minute with a good latch.
- You should no longer feel this pain with latching by four to seven days.
What you can do:
- You can get some relief by rubbing colostrum or breastmilk on your nipples and letting it dry.
- If your nipples continue to be sore, try changing how you hold your baby while breastfeeding, and get help with the latch.
- Pure lanolin products can also help heal nipple pain.
Hot Parent Tip:
If your nipple pain continues throughout the entire feed- you should get help with your latch. Contact your Public Health Nurse or your Health Care Provider. Check out our breastfeeding/chestfeeding resources.
Why do my breasts feel like they are going to explode?
- In the early days of breastfeeding/chestfeeding it is common for your breasts to swell up with milk. This is called engorgement. Your breasts may feel full, heavy and at times be painful.
- Engorgement can also happen after you have been breastfeeding for many weeks if feedings are missed. To avoid this:
- Breastfeed on demand (on baby’s cue) day and night
- Express your milk if you miss a feeding
- If you are starting to wean- do this slowly
Tips for easing engorgement:
- Apply heat (try a warm towel, or disposable diapers filled with warm water or a warm shower) for a couple of minutes and massage your breasts.
- Soften your nipples with your breastmilk, either by hand or with a breast pump (this will make latching easier).
- Make sure your baby is latched on well, and feeds long enough until your breasts feel soft.
- Gently massage your breasts (also called breast compressions) while breastfeeding. This will keep your milk flowing.
- Between feedings, apply cold (cold towels, a diaper soaked in cool water, cabbage leaves) to your breasts for 15-20 minutes. This will help to lessen swelling and pain.
-
If engorgement is not lessened with the above methods:
- Express your breastmilk until you feel comfortable. (by hand, or with a pump)
- Use cold compresses to lessen swelling and pain.
- If necessary, take medications as advised by your health care provider.
Hot parent tips:
- The good news is, engorgement generally only lasts a couple of days.
- Feed your baby at least 8 -12 times in 24 hours, and at least every 3 hours during the day. Continue night feedings.
- As you and your baby learn to breastfeed your body will adapt to meet your baby’s needs.
- Feeding your baby early and often helps to prevent and relieve this discomfort. Feed your baby whenever they shows early feeding cues.
Should I take medications to help increase breast milk?
- Get breastfeeding support if you are having trouble breastfeeding. Personal help can make all the difference. For a list of places that can help, see Breastfeeding resources.
- Domperidone is a prescribed medication that can increase breastmilk supply. It is generally safe and can be effective in increasing breastmilk supply, along with adequate breastfeeding or expressing breastmilk. Speak to your health care provider to see if this medicine is right for you.
- Domperidone can react with other medications so be sure to tell your health care provider that you are using it if you are being prescribed other medications.
- This drug can have some side effects so take only as prescribed. Be sure to taper slowly if you want to stop taking the medication.
- Seek help if you experience mood and or anxiety symptoms anytime before, during or after pregnancy.
Mastitis (breast inflammation):
Mastitis is painful inflammation in the breast tissue which can affect parents who breast/chest feed or exclusively pump. Mastitis can cause pain, swelling, warmth and redness on your breast and can make you feel run down and tired. Some parents may consider weaning their baby sooner then they intended. The good news is you don’t need to wean. You can continue to breastfeed while your mastitis is healing. For more information on mastitis click here.
Plugged Ducts
A tender lump that does not go away with breastfeeding/chestfeeding may be a plugged duct.
What you can do to prevent:
- Breastfeed your baby on demand on both of your breasts
- When unable to breastfeed, express breastmilk at the same frequency you would breastfeed (with a breast pump or by hand).
- Avoid pressure on the area. (wear a comfortable bra, avoid sleeping on the side where you feel pain)
How to treat a plugged duct:
- Apply heat to your breasts for several moments to help soften the plug and help your milk flow. (a warm towel, a clean disposable diaper filled with warm water, a shower)
- Breastfeed your baby on demand on both of your breasts
- When unable to breastfeed, express breastmilk at the same frequency you would breastfeed (with a breast pump or by hand)
- Gently massage the area with your fingertips while you breastfeed
- Hold your baby so his chin and nose points towards the sore area. This will help drain the plugged area. Change positions as needed.
- Contact your health care provider as necessary.

What is a nipple bleb or milk blister?
- A nipple bleb forms because of inflammation of the tissue in the nipple.
- It usually shows up as a painful white or yellowish dot on the nipple or areola.
- If you squeeze your breast, the bleb or blister will typically bulge outward.
- Read our tips on how to manage a nipple bleb or milk blister.
Oral Thrush (Yeast Infections)
Cracked nipples or mastitis can lead to a yeast infection on your nipples.
You may have thrush if you have:
- A shooting, burning pain in the nipple, areola (dark part around your nipple) and breast
- Pain that happens while feeding, even with a good latch, and continues after you breastfeed
- Pinker than usual nipples
- Nipples that are very sensitive to touch
- Nipple cracks that are not healing
Thrush can spread back and forth between you and your baby.

oral thrush on baby’s tongue
Your baby may have thrush if:
- She has small white patchy spots on her tongue, gums and/or roof of mouth that look like milk but do not rub off
- She is fussy while breastfeeding
- She comes on and off your breast while breastfeeding/chestfeeding
- She is gassy and cranky and may have slow gain weight
If you or your baby have any of these signs and symptoms, see your health care provider as soon as possible. You will both need to be treated for yeast infections at the same time. Antifungal creams are used to help clear up thrush.
To prevent reinfection:
- Wash your bras daily and avoid using breast pads if possible.
- If you are using a breast pump, boil the parts daily.
- A soother can carry thrush back into your baby’s mouth, if possible try not to use it and/or replace it frequently. Boil it daily.
What is “tongue-tie”?
Tongue-tie is a fairly common condition that runs in families. It occurs when a thin web of skin under the tongue “ties” the tip of the tongue to the floor of the mouth.
Signs of tongue-tie in the infant include:
- When the tongue looks heart-shaped or notched when stuck out
- Difficulty sticking the tongue out past the lower teeth or up to the upper teeth
- Difficulty moving the tongue from side to side of the mouth
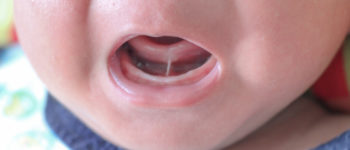
baby with a tongue tie
How a tongue-tie may affect breastfeeding:
- Tongue-tie is a problem for some breastfeeding mothers and babies.
- This is because your baby uses the tongue to get milk from the breast.
- The tongue-tie prevents the baby’s tongue from extending far enough to get a proper latch. This is what can cause a mother to feel pain during breastfeeding.
- Your baby may have trouble getting enough milk out of the breast.
- Mothers often complain about very sore nipples and the baby may be hungry and fussy.
How to treat tongue-tie?
- Sometimes a tongue-tie will stretch over time, allowing the tongue to move better as the baby grows.
- If you have early and ongoing breastfeeding problems, a simple procedure called a frenotomy may free the tongue and help your baby to feed. This procedure can be done on an out-patient basis with minimal if any bleeding or pain.
- Your health care provider can assess the tongue-tie and provide information on where to get frenotomy.
- In Winnipeg, the Pediatric Dentists at Children’s Hospital can perform this procedure if they feel it is necessary. Call 204-787-2516 for information or an appointment.
- This procedure costs about $150. You may be able to claim these costs on your insurance.
References:
Academy of Breastfeeding Medicine Clinical Protocol #36: The Mastitis Spectrum, Revised 2022
Baby’s Best Chance: 7th Edition pages 118-119
- Ballard JL, Auer CE, Khoury JC. (2002). Ankyloglossia: Assessment, incidence and effect of frenuloplasty of the breastfeeding dyad. Pediatrics 110(5): 1-6.
- Griffiths DM. (2004). Do tongue ties affect breastfeeding? Journal of Human Lactation 20(4): 409-414.
- Hogan M, Westcott C, Griffiths M. (2005). Randomized controlled trial of division of tongue-tie in infants with feeding problems. Journal of Pediatric and Child Health 41: 246-250.
- Ricke LA, Baker NJ, Madlon-Kay DJ, DeFor TA. (2005). Newborn tongue-tie: Prevalence and effect on breastfeeding. Journal of American Board Family Practitioners 18(1): 1-7.